All surgeries carry inherent risks. It is the duty of the surgical team and the medical facility to minimize the risks by avoiding errors that result in patient harm. The surgical team should take steps to give the patient the highest level of protection from avoidable surgical mistakes.
Victims can suffer serious consequences when a surgeon or another member of the medical team makes an avoidable error. Such errors could open the door to a medical malpractice claim.
Some actions that are critical for protecting the life and health of a surgery patient – in both hospitals and outpatient surgery facilities – include:
- Follow a fail-safe system to avoid wrong-site surgical errors.
 It is a shocking fact that wrong-site surgeries still occur, as proper procedures could virtually eliminate these events. Any surgical team that relies on handwritten notes or instructions is far more likely to make surgical errors. Human error in entering data in computer systems can also lead to surgical errors, as wrong information may be accessed at several points, including by the surgeon and the attending medical team. Surgical teams must have multiple checks in place to ensure that a wrong-site surgery never occurs. The correct body part must be plainly marked so the surgery site is visible when the patient makes it into the operating room and is not washed off during surgery prep.
It is a shocking fact that wrong-site surgeries still occur, as proper procedures could virtually eliminate these events. Any surgical team that relies on handwritten notes or instructions is far more likely to make surgical errors. Human error in entering data in computer systems can also lead to surgical errors, as wrong information may be accessed at several points, including by the surgeon and the attending medical team. Surgical teams must have multiple checks in place to ensure that a wrong-site surgery never occurs. The correct body part must be plainly marked so the surgery site is visible when the patient makes it into the operating room and is not washed off during surgery prep.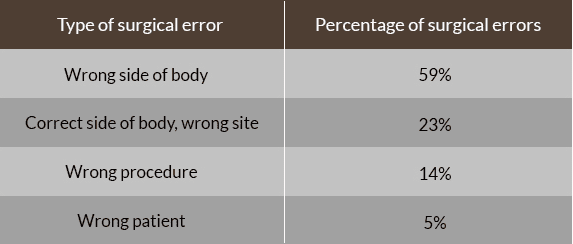
- Hold a pre-operative briefing for the entire team.
 Protocols should include a briefing for all medical professionals involved in the surgery. This helps ensure that each member of the team is focused on the patient, the operation, the expectations, and the team is fully coordinated and in communication – rather than all converging only a few minutes prior to surgery.
Protocols should include a briefing for all medical professionals involved in the surgery. This helps ensure that each member of the team is focused on the patient, the operation, the expectations, and the team is fully coordinated and in communication – rather than all converging only a few minutes prior to surgery. - Don’t rush through the process of pre-op.
 All documentation related to the surgery must be reviewed to ensure that there is no error. The right patient, the right surgery site and any warnings regarding the patient’s medication or medical conditions must all be thoroughly reviewed. Time constraints should not rush the pre-op procedural processes if the risk of a surgical error is to be reduced.
All documentation related to the surgery must be reviewed to ensure that there is no error. The right patient, the right surgery site and any warnings regarding the patient’s medication or medical conditions must all be thoroughly reviewed. Time constraints should not rush the pre-op procedural processes if the risk of a surgical error is to be reduced. - Take a time-out for verification.
 The surgical team should have a “time-out” before starting the operation to verify critical issues such as right patient, right procedure and right surgical site before beginning the surgery.
The surgical team should have a “time-out” before starting the operation to verify critical issues such as right patient, right procedure and right surgical site before beginning the surgery. - All members of the surgical team must be well-rested.
 A tired surgeon, anesthesiologist, nurse or other member of the surgical team is more likely to make an error that could be serious or even fatal. The entire surgical team must ensure that they are well-rested before doing anything in the operating room.
A tired surgeon, anesthesiologist, nurse or other member of the surgical team is more likely to make an error that could be serious or even fatal. The entire surgical team must ensure that they are well-rested before doing anything in the operating room. - Do one thing at a time to avoid retained foreign objects.
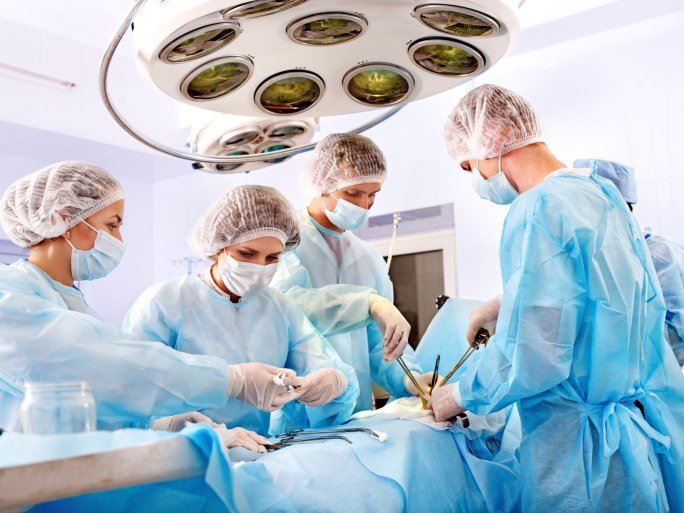 Multi-tasking on the part of the surgical team is one of the most common reasons that surgical instruments, sponges and other foreign objects are left inside the body of patients. For example, a nurse may count surgical instruments while the surgeon is still in the final steps of surgery, leading to a miscount. When attention is required for several different actions, there is a greatly increased risk of a surgical error involving a retained foreign object.
Multi-tasking on the part of the surgical team is one of the most common reasons that surgical instruments, sponges and other foreign objects are left inside the body of patients. For example, a nurse may count surgical instruments while the surgeon is still in the final steps of surgery, leading to a miscount. When attention is required for several different actions, there is a greatly increased risk of a surgical error involving a retained foreign object. - Allow no distractions in the operating room.
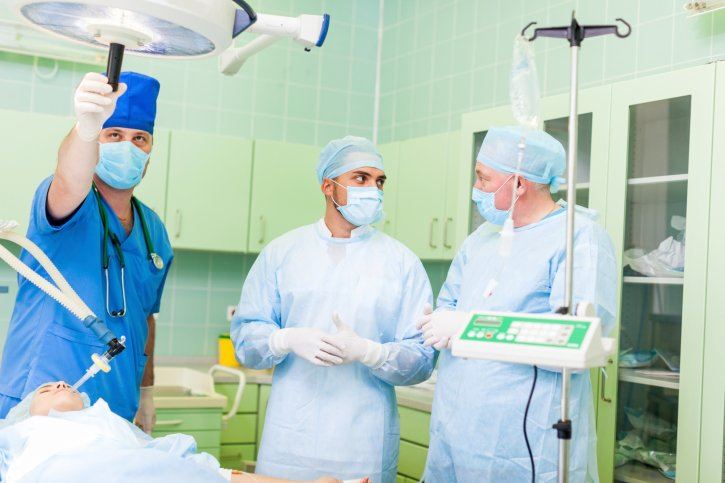 Chatting among personnel, music playing or other forms of distraction can greatly increase the risk of an error. It only adds to the problem when people enter and leave the operating room, asking questions of the various medical professionals who are taking part in the surgery. This is a particular problem when instruments are being counted. Concentration on the task at hand is crucial in an effort to avoid the risk of a serious surgical error.
Chatting among personnel, music playing or other forms of distraction can greatly increase the risk of an error. It only adds to the problem when people enter and leave the operating room, asking questions of the various medical professionals who are taking part in the surgery. This is a particular problem when instruments are being counted. Concentration on the task at hand is crucial in an effort to avoid the risk of a serious surgical error. - Beware of X-ray flips.
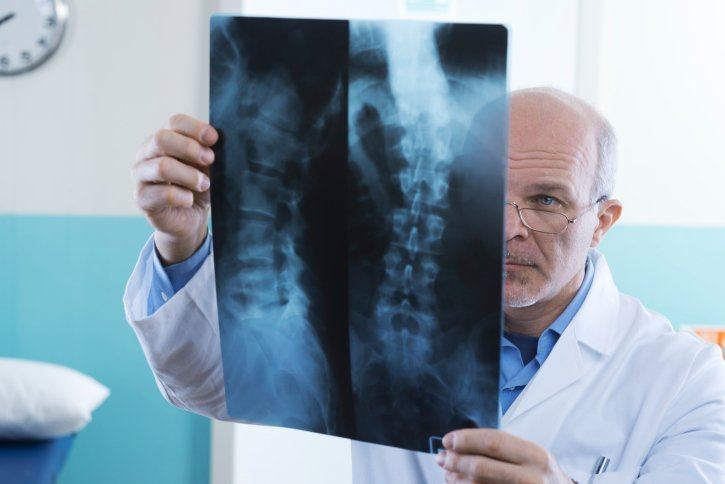 An X-ray that is viewed from the wrong side may lead to a wrong-side surgical error. Every detail about the patient must be evaluated to determine if there is conflicting information about which side of the body the surgery is to be performed on. Rushing through the process may lead to an error that could be fatal or lead to long-term complications.
An X-ray that is viewed from the wrong side may lead to a wrong-side surgical error. Every detail about the patient must be evaluated to determine if there is conflicting information about which side of the body the surgery is to be performed on. Rushing through the process may lead to an error that could be fatal or lead to long-term complications.
The Cost of Medical Mistakes
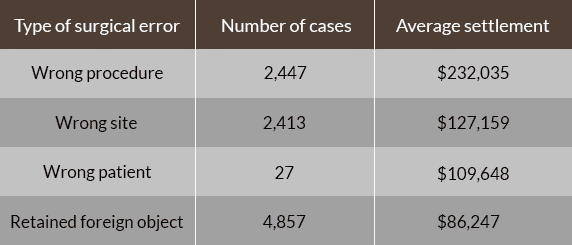
The value of a malpractice settlement varies based on many factors. Research into the value of medical liability settlements from 1990-2010 reveals the high cost of surgical errors. Settlements reached as high as $7.1 million.
This chart reflects only the average of all payouts to victims for an act of medical negligence during those years.
Sources:
- Agency for Healthcare Research and Quality – Patient Safety Primers: Wrong-Site, Wrong-Procedure, and Wrong-Patient Surgery
- The Joint Commission – Wrong Site Surgery Resources and Sentinel Event Alerts about Wrong Site Surgery
- American Medical News – Surgical errors: In ORs, “never events” occur 80 times a week









